Table of Contents
1. Clinical Assessment
History
- Onset, duration, frequency, and number of ulcers
- Pain severity, triggers (trauma, stress, certain foods)
- Systemic symptoms: fever, diarrhea, joint pain, fatigue
- Family history of similar lesions
- Medications (NSAIDs, beta-blockers)
- Previous treatments and response
Examination
- Location: non-keratinized mucosa (buccal, labial, ventral tongue, floor of mouth)
- Size:
- Minor (<1 cm) – most common
- Major (>1 cm, deeper, may scar)
- Herpetiform (multiple small ulcers)
- Number: single or multiple
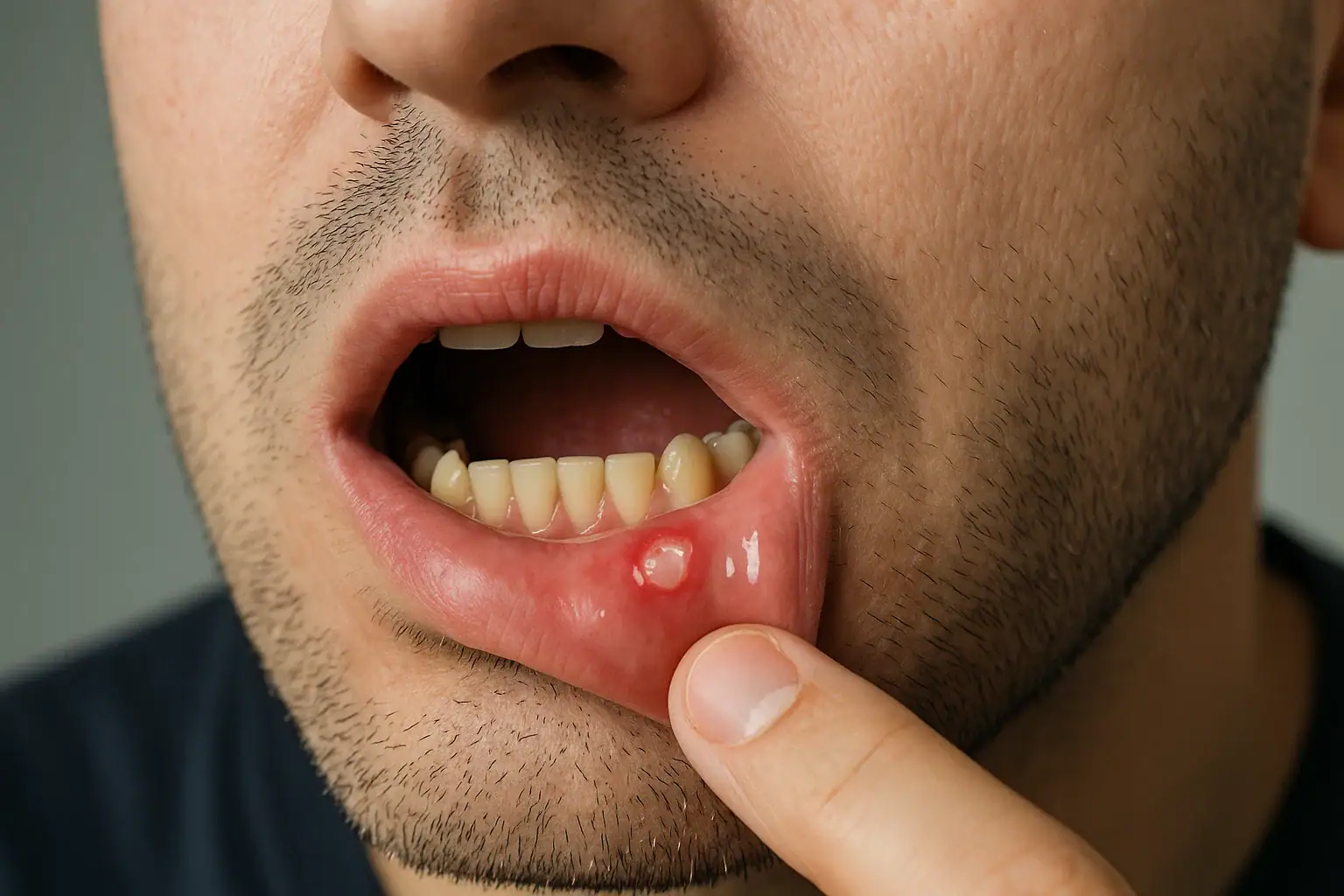
- Appearance: round/oval, yellow-white pseudomembrane with erythematous halo
- Rule out: secondary causes (herpes simplex, trauma, systemic disease)
2. Investigations (If atypical or recurrent)
- Basic labs: CBC, iron studies, vitamin B12, folate (nutritional deficiencies)
- CRP/ESR: if systemic symptoms
- Serology: celiac disease (tTG-IgA), HIV (if risk factors)
- Biopsy: rare, only if persistent >3 weeks, atypical, or suspected malignancy
- Microbiology: rarely needed; ulcers are typically non-infectious
3. Classification
| Type | Features | Management Focus |
|---|---|---|
| Minor | <1 cm, 1–5 lesions, heal 7–14 days | Symptomatic relief |
| Major | >1 cm, deep, persistent, may scar | Systemic therapy possible |
| Herpetiform | Multiple, small, coalescing, painful | Combination topical/systemic therapy |
4. Management
A. General Measures
- Avoid triggers: spicy/acidic foods, trauma
- Good oral hygiene
- Avoid sodium lauryl sulfate in toothpaste
- Stress management
- Nutritional supplementation if deficient
B. Topical Therapy (First-line for minor ulcers)
- Topical corticosteroids:
- Triamcinolone acetonide 0.1% in orabase
- Fluocinonide 0.05% gel
- Topical anesthetics:
- Lidocaine 2% gel for pain relief
- Protective agents:
- Orabase, hydroxypropyl cellulose films
C. Systemic Therapy (For severe, recurrent, or major ulcers)
- Oral corticosteroids:
- Prednisone short course (e.g., 30–60 mg/day tapering)
- Immunomodulators (refractory cases):
- Colchicine, thalidomide, dapsone
- Address underlying systemic disease:
- Nutritional deficiencies, IBD, Behçet’s disease, etc.
D. Adjunctive Therapy
- Antimicrobial mouth rinses: chlorhexidine gluconate
- Pain control: NSAIDs (if not contraindicated)
- Laser therapy (experimental for pain reduction and healing)
5. Follow-Up
- Minor ulcers: usually self-limiting; review if >3 weeks
- Recurrent or major ulcers: monitor frequency, severity, and response to therapy
- Evaluate for systemic disease if persistent or atypical