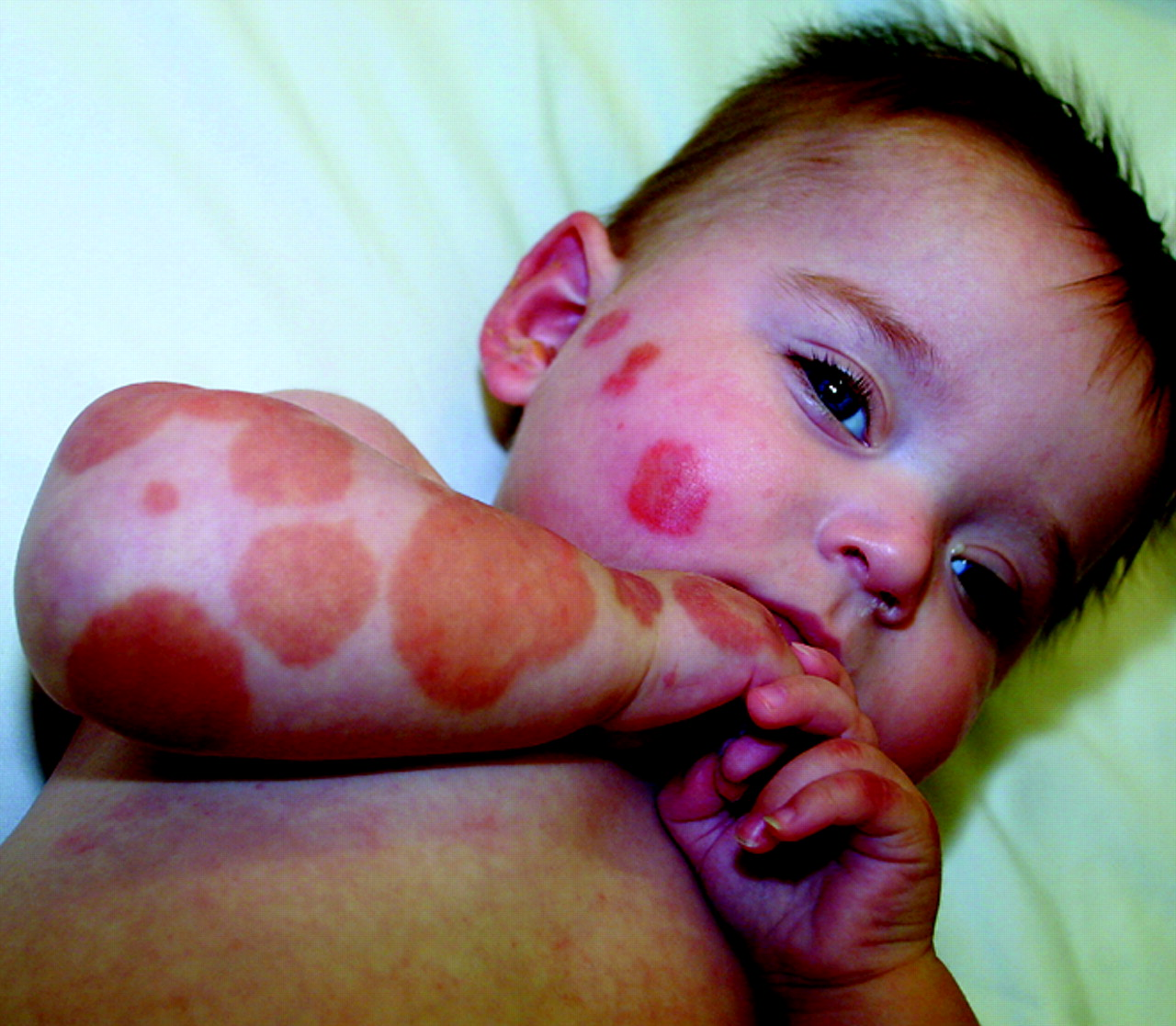
Acute Haemorrhagic Edema of Infancy
The alarming rash that almost always gets better on its own — a deep dive for parents, students, and curious clinicians.
In this article
“A toddler in your clinic has enormous, coin-shaped bruise-like patches spreading across her cheeks and limbs. Her parents are terrified. But she is smiling, playing, and completely unconcerned. What is going on?”
When the rash looks worse than it is
Acute Haemorrhagic Edema of Infancy (AHEI) — also written as AHEi, and known in older texts as Finkelstein’s disease or Seidlmayer syndrome — is one of medicine’s most dramatic-looking but ultimately benign conditions. It is a small-vessel vasculitis affecting infants, producing spectacular purpuric and ecchymotic (bruise-like) plaques that arrive almost overnight, often sending terrified caregivers rushing to emergency departments.[1,2]
The condition was first described by Seidlmayer in 1939 and by Snow in 1913, though Finkelstein had noted similar cases even earlier in 1894. Despite a century of literature, AHEI is still frequently mistaken for more ominous diagnoses — septicaemia, Henoch–Schönlein Purpura (HSP), child abuse, or meningococcal disease — because the skin findings look so alarming.[3]
Who gets it — and when
(months)
ratio
full resolution
rate
AHEI predominantly affects infants between 4 months and 2 years of age, with the highest incidence between 4 and 24 months. Cases outside this range have been reported, but they are rare. A mild male predominance (roughly 2:1) has been noted in several case series.[4]
The condition is not truly rare — it is underreported and underdiagnosed. In a retrospective review by Fiore et al. (2008), AHEI accounted for a significant proportion of leukocytoclastic vasculitis referrals in the paediatric age group when looked for specifically.[5]
Common preceding events identified in the literature include:
- Upper respiratory tract infections (most common)
- Otitis media
- Urinary tract infection
- Vaccinations (MMR, DTP, meningococcal)
- Antibiotic use (amoxicillin being most frequently implicated)
- Insect bites (less commonly)
What is happening inside the skin
AHEI is classified as a leukocytoclastic vasculitis — a pattern of small-vessel inflammation where neutrophils infiltrate and destroy vessel walls, leaving behind debris (“nuclear dust”). The immune mechanism involves deposition of immune complexes (antigen–antibody complexes) in the walls of small dermal blood vessels, triggering complement activation and neutrophil recruitment.[6]
Immunofluorescence studies have demonstrated IgA, IgM, C3, and fibrinogen deposition in vessel walls in some cases, though IgA deposition — the hallmark of HSP — is inconsistent and when present is usually less prominent than in HSP.[3,7]
“The pathological findings in AHEI may be indistinguishable from those of Henoch–Schönlein purpura on routine histology, yet the clinical course is entirely different — strikingly self-limited and benign.” — Bolognia, Schaffer & Cerroni (2018)[6]
The absence of systemic organ involvement (kidney, gut, joints) despite florid skin vasculitis remains intriguing. Current thinking suggests that in AHEI, the immune complex insult is limited to the dermis, without the IgA-dominant, multisystem involvement that characterises HSP. The specific antigen driving immune complex formation is usually never identified, though viral antigens are presumed in most cases.
The diagnostic triad
The clinical presentation of AHEI is almost pathognomonic — once seen, it is hard to forget. The classic triad, described by Legrain et al. (1991), consists of:[8]
The cockade or medallion morphology of the plaques is characteristic: purpuric patches with concentric rings of varying colour (red, purple, and brown), resembling a target or rosette. Lesions range from 1–5 cm and are most densely distributed on the face, ears (pinna involvement is classic), and lower limbs. The trunk is notably spared in most cases.[1,4]
Mucous membranes are typically spared. The child, despite looking florid and alarming on the surface, is usually playful, feeding well, and in no systemic distress — a crucial clinical observation. This dissociation between frightening appearance and well general state is one of the most important pointers to AHEI.
Telling it apart from HSP and other mimics
The single greatest diagnostic challenge in AHEI is distinguishing it from Henoch–Schönlein Purpura (IgA vasculitis), as both cause purpuric rashes in young children following infections. The table below summarises key distinguishing features:[1,2,3,6]
| Feature | AHEI | HSP (IgA Vasculitis) |
|---|---|---|
| Age | 4 months – 2 years | 3 – 10 years (peak) |
| Rash morphology | Cockade/medallion ecchymotic plaques | Palpable purpura, petechiae |
| Distribution | Face, ears, limbs (trunk spared) | Lower limbs and buttocks (symmetric) |
| Oedema | Prominent facial/acral | Mild, less prominent |
| Arthritis/arthralgia | Absent | Present in ~75% |
| Renal involvement | Absent (very rare case reports) | Present in ~40–50% |
| GI involvement | Absent | Present in ~60% |
| IgA deposition (DIF) | Inconsistent / absent | Prominent (diagnostic) |
| Resolution | 1–3 weeks | Weeks to months |
| Recurrence | Rare (<5%) | Up to 33% |
Other important differentials include:
- Urgent Meningococcal / bacterial septicaemia — unwell child, high fever, rapidly progressive
- Urgent Child abuse / non-accidental injury — pattern assessment, safeguarding history
- Consider Erythema multiforme — targetoid but less haemorrhagic; mucous membrane involvement
- Consider Urticaria multiforme — wheals, no true purpura, dermatographism
- Less urgent Drug hypersensitivity reactions
- Less urgent Sweet syndrome — rarer; neutrophilic, elevated inflammatory markers
How doctors confirm the diagnosis
AHEI is primarily a clinical diagnosis. In a well-appearing infant with the characteristic triad — cockade purpura on the face, ears, and limbs; facial oedema; low-grade fever — no further testing is strictly required if the child is clinically stable.[1,3]
However, in practice, investigations are often performed to exclude more serious diagnoses, especially at the first presentation. Typical findings include:
- Full blood count: Usually normal or mild leukocytosis. Platelets normal — this is key to ruling out thrombocytopaenia-related purpura.
- Coagulation screen: Normal PT and APTT distinguish AHEI from DIC or coagulopathy.
- CRP / ESR: Mildly elevated or normal.
- Renal function / urinalysis: Normal — no haematuria or proteinuria (differentiates from HSP nephritis).
- Blood culture: Negative (performed to exclude septicaemia).
- Serum IgA: Normal or slightly elevated; not consistently elevated as in HSP.
Management — less is more
This is where AHEI stands apart from most paediatric vasculitides: no specific treatment is required. The cornerstone of management is reassurance — to the family and to the clinical team.[1,2]
The following principles guide management:
- Watchful waiting: Lesions resolve spontaneously in 1–3 weeks without treatment in the vast majority of cases.
- Corticosteroids: Not routinely indicated. Some authors have used short courses of oral prednisolone for severe or prolonged cases, but there is no strong evidence base. Garty et al. and others have noted that steroids do not significantly alter the course.[9]
- Antihistamines: May be used for symptomatic comfort if itching is present, though the rash is not typically pruritic.
- Identify and treat triggers: If an underlying infection (e.g., otitis media) prompted the reaction, treat it appropriately.
- Avoid unnecessary admissions: A well-looking child with a clear clinical picture can be managed as an outpatient with clear safety-netting advice.
Hospitalisation may be appropriate for the first episode when the diagnosis is uncertain, to perform investigations and observe the child’s trajectory. Once diagnosis is confirmed and the child is shown to be systemically well, outpatient follow-up is sufficient.
Prognosis and follow-up
The prognosis of AHEI is excellent. In the landmark review by Legrain et al. (1991) and subsequent series, virtually all cases resolved without sequelae.[8] Skin lesions fade over 1–3 weeks, typically without post-inflammatory hyperpigmentation or scarring. The oedema resolves in parallel.
Recurrence is uncommon, reported in fewer than 5% of cases, usually following another triggering infection. Chronic or recurring AHEI should prompt reassessment of the diagnosis — particularly to reconsider HSP or other vasculitides.[3]
Renal involvement has been reported in isolated case reports but is sufficiently rare that routine long-term renal follow-up is not warranted unless urinalysis is abnormal at presentation.[1,5]
References
- 1Tlougan BE, Podjasek JO, O’Haver J, Cordova KB, Nguyen XH, Tee R, Hansen RC. Acute hemorrhagic edema of infancy (AHEI): a practice-based approach. Pediatric Dermatology. 2013;30(2):222–229.
- 2Paller AS, Mancini AJ. Hurwitz Clinical Pediatric Dermatology. 5th ed. Philadelphia: Elsevier; 2016. pp.505–506.
- 3Waskerwitz S, Christodoulou J. Finkelstein’s disease (acute hemorrhagic edema of infancy). In: Irvine AD, Hoeger PH, Yan AC, eds. Harper’s Textbook of Pediatric Dermatology. 3rd ed. Oxford: Wiley-Blackwell; 2011. Chapter 56.
- 4Kraft JN, Frieden IJ. Vascular reactions: urticaria, erythema multiforme, and drug hypersensitivity reactions. In: Eichenfield LF, Frieden IJ, Esterly NB, eds. Neonatal Dermatology. 2nd ed. Philadelphia: Saunders; 2008.
- 5Fiore E, Rizzi M, Ragazzi M, Vanoni F, Bernasconi M, Bianchetti MG, Simonetti GD. Acute hemorrhagic edema of young children (cockade purpura and edema): a case series and systematic review. Journal of the American Academy of Dermatology. 2008;59(4):684–695.
- 6Callen JP, Mancini AJ. Cutaneous vasculitis. In: Bolognia JL, Schaffer JV, Cerroni L, eds. Dermatology. 4th ed. Philadelphia: Elsevier; 2018. Chapter 24.
- 7Mancini AJ, Shani-Adir A. Other viral diseases. In: Bolognia JL, Schaffer JV, Cerroni L, eds. Dermatology. 4th ed. Elsevier; 2018.
- 8Legrain V, Lejean S, Taieb A, Guillard JM, Battin J, Maleville J. Infantile acute hemorrhagic edema of the skin: study of ten cases. Journal of the American Academy of Dermatology. 1991;24(1):17–22.
- 9Garty BZ, Poznanski O. Acute hemorrhagic edema of infancy. Israel Medical Association Journal. 2000;2:546–547.
- 10Trapani S, Mariotti P, Resti M, Nappini L, De Martino M, Falcini F. Severe hemorrhagic bullous lesions in Henoch-Schönlein purpura: three paediatric cases and review of the literature. Rheumatology International. 2010;30(8):1063–1067.
- 11Burns T, Breathnach S, Cox N, Griffiths C, eds. Rook’s Textbook of Dermatology. 9th ed. Oxford: Wiley-Blackwell; 2016. Chapter on vasculitis.